|
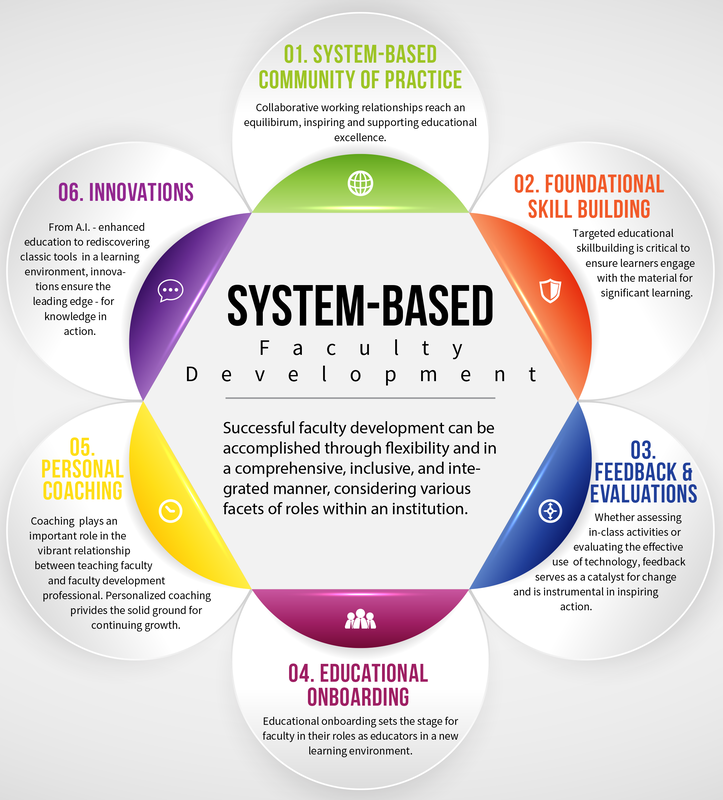
Implementing a new faculty development program is exciting! However, the multifaceted nature of faculty development comes with many questions, e.g., how to provide value to the faculty within a unique professional environment and culture, how to inspire innovation and growth, and how the institutional community can collaborate to take ownership of their own growth, for the benefit of learners? “Faculty development refers to all activities health professionals pursue to improve their knowledge, skills and behaviors as teachers and educators, leaders and managers, and researchers and scholars, in both individual and group settings.” (1) Ideally, the most effective faculty development programs are those that focus on ongoing and communicative partnerships among faculty, staff, and school leadership, where colleagues actively engage in their own development and are fully supported by mentors. These programs should be multifaceted, including the identification and achievement of teaching performance goals, participation in discipline-specific activities, and membership in professional organizations. Faculty development approaches may comprise various strategies to enhance educators' skills and knowledge. These approaches include online learning, peer coaching, workshops, seminars, fellowships, and longitudinal programs. They may be structured and implemented in various ways and encompass a variety of engagement and rigor, ranging from competency-based to immersive and experiential, using both traditional cultural approaches or new technologies such as simulation and AI. In general, interpersonal relationships and psychological safety are valued, and coaching as an emerging framework for professional development is key for individual needs, as is creating communities of practice, fostering shared learning and collaboration among faculty. (2)(3)(4)(5) I would like to address a system-based faculty development framework that includes key elements continually emerging from my practical experience. These key elements include (1) Communities of Practice; (2) Foundational Skill Building; (3) Feedback & Evaluations; (4) Educational Onboarding; (5) Personal Coaching; and (6) Innovations.  One key aspect is the formation of Communities of Practice (CoP), which involve shared interests, practices, and resources among members over time. Communities of practice (CoP) for faculty development offer an effective and sustainable approach for knowledge management and implementation of best practices. A successful CoP creates and shares knowledge in the context of a specific practice toward the development of expertise. Their collaborative nature, based on the co-creation of practical solutions to daily problems, aligns well with the goals of applying best practices in health professions education and training new faculty members. CoPs can be facilitated through technology and offer benefits like sharing best practices and creating a supportive network. (6)(7)(15)  Foundational skill-building in faculty development focuses on improving a broad range of skills, including teaching, leadership, research, or clinical skills through reflection, observation, and hands-on learning experiences. As an example, competency-based skill building such as, e.g., conducting active teaching and learning in learning sessions, requires role-modeling for optimizing learning. Building foundational skills in various forms is often closely aligned with an organization's vision and mission, reflecting its educational culture. (8)  Effective faculty development programs benefit from key features such as experiential learning, feedback provision, strong peer and colleague relationships, well-designed interventions based on teaching and learning principles, and variety of educational methods. Feedback and evaluations are invaluable in faculty development, serving as essential tools for refining teaching practices, enhancing skills, and aligning goals with student needs and institutional requirements. Effective feedback in faculty development not only identifies strengths and areas for improvement but also guides professional growth and fosters a culture of continuous learning. It empowers faculty to refine their teaching strategies, understand their performance, and ultimately thrive in their roles. (9)  As foundational as an institution's vision and mission are, so, too, is the importance of educational onboarding. Educational onboarding in faculty development can be an exciting process that offers personalized experiences, comprehensive orientations, and valuable connections to resources, as well as an immersion into a new educational culture. Besides clear expectations, networking opportunities, and promotion pathways, onboarding is uniquely tailored to accommodate the diverse job functions tied to specific times, like the beginning of a semester. For instance, facilitating the sharing of educational resources is crucial to ensure the new faculty's success. Designing unique onboarding experiences not only speeds up integration of the new faculty but also allows introspection in its own unique procedures, purpose, or identity. (10). Innovative, excellent approaches may, e.g., include videos featuring leadership and faculty introducing departments, faculty, and processes, and welcoming new faculty.  Coaching in faculty development is incredibly valuable, providing a personalized, safe space that enhances teaching effectiveness and fosters professional success. The coaching model in medical and health professions education prioritizes the role of faculty members as coaching participants, ensuring that their needs and goals are at the forefront. This approach has proven to be particularly effective in improving teaching skills and feedback effectiveness, with simulated student scenarios serving as a successful coaching strategy. The American Medical Association's coaching handbook for medical education faculty underscores the importance of separating content knowledge from skills. It emphasizes using small group settings for skill building through experiential learning activities, which has been shown to be highly effective. Overall, coaching in faculty development offers significant benefits for both faculty and students. In my experience, individualized coaching provides tailored solutions that complement the broader educational programs, enhancing the overall learning experience. (11) (12) (13) (15) And finally.... Innovation stands at the forefront of faculty development for health professions education, igniting advancements in curriculum, research, and student engagement, oftentimes as a response to urgent emerging problems. The rise of technology-enhanced faculty development presents a wealth of opportunities for both experience and scholarship, including access to diverse devices; instant feedback mechanisms; enhanced education accessibility through online models, apps, and blogs; and enhanced experience through artificial intelligence. Successful implementation requires careful planning to achieve desired outcomes while seamlessly integrating into faculty practices. (14) (15) Overall, effective faculty development programs are grounded in experiential learning, enriched by effective feedback mechanisms, informed by peer-reviewed concepts, diverse educational strategies, and unique institutional cultures. These programs are instrumental in fostering Continuous Professional Development (CPD) across a spectrum of skills. Regular evaluation is pivotal, and embracing innovative technologies can elevate learning experiences for both students and faculty, ushering in a new era of educational excellence. References: (1) Steinert, Y. (Ed.). (2014). Faculty development in the health professions: A focus on research and practice (Vol. 11). Springer Science & Business Media. (2) de Carvalho-Filho, M. A., Tio, R. A., & Steinert, Y. (2020). Twelve tips for implementing a community of practice for faculty development. Medical teacher, 42(2), 143-149. (3) Guraya, S. Y., & Chen, S. (2019). The impact and effectiveness of faculty development program in fostering the faculty’s knowledge, skills, and professional competence: A systematic review and meta-analysis. Saudi journal of biological sciences, 26(4), 688-697. (4) Devassy, S. M., Scaria, L., Metzger, J., Thampi, K., Jose, J., & Joseph, B. (2023). Development of immersive learning framework (ILF) in achieving the goals of higher education: measuring the impact using a pre–post design. Scientific Reports, 13(1), 17692. (5) Kohan, M., Changiz, T., & Yamani, N. (2023). A systematic review of faculty development programs based on the Harden teacher’s role framework model. BMC Medical Education, 23(1), 910. (6) Wenger, E. (1998). Communities of Practice: Learning, Meaning and Identity. New York: Cambridge University Press. (7) Fornari, A. (no date). Nurturing Faculty Development Programs to Guide The Formation of Communities of Practice. [Slide Set] accessed April 4, 2024. https://medicine.hofstra.edu/pdf/faculty/facdev/facdev-prodev-copworkshop.pdf (8) Padilla, L., Garcia, D. T., Rodrigues, A., & Hyun, M. (2022). Training for the future: Introducing foundational skills necessary to promote patient-centered care practice in medical physics graduate programs. Technical Innovations & Patient Support in Radiation Oncology, 24, 54-58. (9) Steinert, Y., Mann, K., Centeno, A., Dolmans, D., Spencer, J., Gelula, M., & Prideaux, D. (2006). A systematic review of faculty development initiatives designed to improve teaching effectiveness in medical education: BEME Guide No. 8. Medical teacher, 28(6), 497-526. (10) Roberts-Lieb, S. & Best, R. G. (2024). Starting on the Right Foot: Faculty Onboarding With a Purpose https://www.aamc.org/professional-development/affinity-groups/gfa/faculty-onboarding-purpose (11) Branzetti J (2023). MD MHPE Coaching for Faculty: The Secret to Unlocking Professional Success. [blog post]. https://www.aliem.com/coaching-faculty-secret-unlocking-professional-success/ (12) Orr, C. J., & Sonnadara, R. R. (2019). Coaching by design: Exploring a new approach to faculty development in a competency-based medical education curriculum. Advances in medical education and practice, 229-244. (13) Hammoud, M. M., Deiorio, N. M., Moore, M., & Wolff, M. (2022). Coaching in Medical Education: Coaching in Medical Education-E-Book. Elsevier Health Sciences. (14) Yilmaz, Y., Lal, S., Tong, X. C., Howard, M., Bal, S., Bayer, I., ... & Chan, T. M. (2020). Technology-enhanced faculty development: future trends and possibilities for health sciences education. Medical science educator, 30, 1787-1796. (15) Steinert, Y., O’Sullivan, P. S., & Irby, D. M. (2023). The Role of Faculty Development in Advancing Change at the Organizational Level. Academic Medicine, 10-1097. Would you like to learn more? Contact me! Email: [email protected]
2 Comments
|